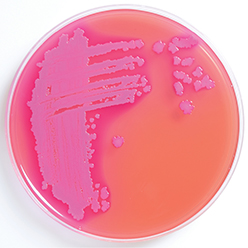
"blood agar." It is a type of microbiological culture medium used for cultivating bacteria. It consists of agar, a solidifying agent, and animal blood, typically from sheep, horse, or cattle. The blood is added to the medium to provide additional nutrients for the growing bacteria.
This type of medium is often used to detect the presence of hemolytic bacteria, which can lyse the red blood cells present in the blood. The three main types of observed hemolysis are alpha (partial) hemolysis, beta (complete) hemolysis, and gamma (no hemolysis) hemolysis. These hemolysis characteristics can aid in identifying different types of pathogenic bacteria.
Blood agar plates are widely used in medical laboratories for diagnosing bacterial infections and for testing bacteria's susceptibility to antibiotics.
Application
- Isolation and Identification of Pathogens: Blood agar plates are commonly used in clinical microbiology laboratories to isolate and identify pathogenic bacteria from patient samples such as blood, urine, wounds, and respiratory secretions. The blood in the agar provides nutrients that support the growth of a wide range of bacteria, allowing for the isolation of various pathogens.
- Detection of Hemolytic Activity: Blood agar plates are particularly useful for detecting hemolytic activity exhibited by certain bacteria. When cultured on blood agar, some bacteria produce enzymes (hemolysins) that can lyse red blood cells, resulting in distinct patterns of hemolysis around the bacterial colonies. This characteristic hemolysis pattern can aid in the preliminary identification of bacterial species and in distinguishing between different types of hemolytic bacteria.
- Identification of Streptococci: Blood agar plates are essential for identifying and differentiating various species of streptococci based on their hemolytic properties. Streptococci are categorized into three groups based on their hemolysis patterns on blood agar: alpha-hemolytic (partial hemolysis), beta-hemolytic (complete hemolysis), and gamma-hemolytic (no hemolysis). This classification helps in diagnosing streptococcal infections and determining appropriate treatment strategies.
- Antimicrobial Susceptibility Testing: Blood agar plates can also be used for antimicrobial susceptibility testing to determine the effectiveness of antibiotics against bacterial isolates. After culturing bacteria on blood agar, antibiotic discs are placed on the surface of the agar, and the zones of inhibition around the discs are measured to assess bacterial susceptibility to specific antibiotics. This information guides clinicians in selecting the most appropriate antimicrobial therapy for treating bacterial infections.
Overall, blood agar plates play a crucial role in clinical microbiology by facilitating the isolation, identification, and characterization of pathogenic bacteria, as well as aiding in antimicrobial susceptibility testing for effective patient management.